Muscle Loss & Sarcopenia: How Aging Steals Strength and Energy

muscle loss and sarcopenia: the silent process that reshapes strength, mobility, and aging
Muscle loss and sarcopenia can start earlier than most people think. They often begin quietly in midlife. You may notice smaller changes first. You get tired faster. Stairs feel harder. Balance feels less stable. These signs matter because skeletal muscle supports daily movement, stable blood sugar, and long-term independence.
Sarcopenia describes the age-related drop in muscle mass, muscle strength, and physical performance. Aging plays a role, but lifestyle drives a large part of the curve. Long sitting hours, low protein intake, poor sleep, and low-grade inflammation can speed muscle decline. The good news is simple: muscle still responds to smart training, better nutrition, and better recovery at any age.
This pillar guide explains muscle loss and sarcopenia in clear, evidence-based terms. You will learn what they are, why they happen, and what strategies research supports. You will also learn who should move carefully and which mistakes often backfire.
why muscle loss matters more than most people realize
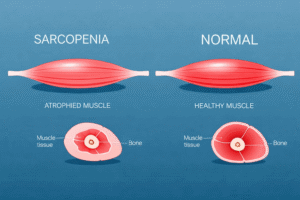
Skeletal muscle does much more than move the body. It acts like a metabolic organ. It helps clear glucose from the blood after meals. It supports insulin sensitivity. It also influences inflammation and energy use. When you lose muscle, you often lose metabolic resilience at the same time.
Long-term research links low muscle strength with falls, frailty, and loss of independence. Strength often predicts function better than body weight does. That is why “normal weight” does not always mean “low risk.” Muscle quality and strength matter.
what is sarcopenia?
Sarcopenia is the progressive loss of skeletal muscle mass and strength, along with reduced physical performance. Clinicians often assess it using measures like grip strength, chair-rise ability, and walking speed. Muscle strength can drop faster than muscle size. So people may look “the same” while function declines.
For a concise clinical overview, see the NIH/NCBI reference on sarcopenia here:
Sarcopenia (NIH NCBI Bookshelf).
a short historical and lifestyle perspective
Humans evolved with daily physical demand. We walked, carried, climbed, and lifted. That constant loading helped preserve muscle across life. Modern life often removes those signals. We sit for long blocks of time. We drive short distances. We avoid heavy effort. Over years, muscle “learns” it is not needed as much.
This matters because sarcopenia is not only about age. It is also about input. The body adapts to what you ask it to do.
the biology behind muscle loss and sarcopenia
Muscle mass depends on balance. You build muscle through muscle protein synthesis. You lose muscle through muscle protein breakdown. When synthesis stays higher, muscle holds steady or grows. When breakdown stays higher, muscle shrinks.
With age, several forces can shift the balance:
- anabolic resistance, which means aging muscle responds less to protein
- lower anabolic hormones over time
- chronic low-grade inflammation
- less mechanical loading from inactivity
Anabolic resistance is central. Older muscle often needs a stronger signal. That signal comes from protein, strength training, and recovery working together.
muscle, nerves, and “strength that disappears first”
Strength depends on muscle fibers and the nervous system. The brain must recruit fibers fast and efficiently. With age, some motor units weaken or drop out. Fast-twitch fibers also decline more than slow-twitch fibers in many people. That can reduce power and balance correction. This helps explain why falls become more likely, even when pain is not present.
when does muscle loss usually begin?
Many adults reach peak muscle mass around early adulthood and midlife. After that, muscle loss can start gradually. The pace varies a lot. Activity level, protein intake, health conditions, and long inactivity periods all matter. A short illness or injury can cause a fast drop. That is why prevention in midlife pays off.
For a public-health overview of sarcopenia and aging muscle, see:
NIH News in Health: Slowing Sarcopenia.
muscle loss versus weight loss
People often assume muscle loss happens only when body weight drops. That is not true. You can lose muscle while body weight stays the same. This can happen when fat mass rises as muscle declines. Some call this pattern sarcopenic obesity. It can raise risk because function drops while metabolic strain rises.
If you want fat loss later in life, you must protect muscle at the same time. That usually means adequate protein, resistance training, and a modest calorie deficit. Extreme dieting often costs muscle.
muscle loss, insulin resistance, and metabolic aging
Muscle loss and sarcopenia connect tightly to metabolic aging. Skeletal muscle is the main site for glucose uptake after meals. When muscle mass and muscle quality drop, the body has fewer “storage and use” sites for glucose. Blood sugar can rise for longer. The pancreas often responds by producing more insulin.
Over time, this pattern can support insulin resistance. This link can appear even in people who do not have obesity. Muscle health helps set the floor for metabolic health.
why muscle acts like a metabolic organ
Active muscle releases myokines. These signals can support insulin sensitivity and help regulate inflammation. Less muscle activity often means less helpful signaling. At the same time, excess fat tissue can increase inflammatory signaling. The combination can speed metabolic decline.
why sitting time can undermine progress
Long sitting blocks can reduce insulin sensitivity. This can happen even in people who exercise. Simple breaks help. Stand up. Walk for a few minutes. Do light leg work. These small actions send a signal that muscle is still needed.
muscle loss, mitochondrial health, and aging energy
Many people describe aging as “low energy.” Often, muscle biology sits under that feeling. Muscle cells contain mitochondria. Mitochondria help produce cellular energy. When mitochondrial function drops, muscles fatigue sooner and recover more slowly.
Aging can reduce mitochondrial efficiency, but lifestyle also shapes it. Inactivity, poor sleep, and metabolic stress can worsen the decline. Strength training and regular movement can improve mitochondrial signaling and support healthier energy use over time.
why mitochondria matter for muscle building
Muscle repair and growth require energy. Amino acid transport, tissue rebuilding, and recovery all use ATP. When energy production runs low, the body may struggle to rebuild efficiently. That can shift balance toward breakdown.
nutrition strategies for muscle protein synthesis
Nutrition supports muscle in two main ways. It provides amino acids for repair. It also provides energy for recovery and training. For muscle loss and sarcopenia, protein quality, protein timing, and total intake all matter.
protein: amount and distribution across the day
Many people eat very little protein early in the day and a lot at dinner. That pattern can limit muscle protein synthesis. A steadier distribution across meals often works better for aging muscle. It gives repeated “build” signals instead of one late spike.
High-quality proteins that contain all essential amino acids help. Leucine-rich options often provide a stronger muscle-building signal. Whole foods can cover this in many cases.
For a practical, evidence-based overview of protein needs and sarcopenia, see:
Harvard Health: Muscle loss and protein needs in older adults.
do not starve the system during weight loss
Aggressive calorie restriction can speed muscle loss, especially with low protein. If your goal includes fat loss, keep the deficit modest and keep protein adequate. Pair it with resistance training. This approach helps protect lean mass while weight trends down.
key nutrients that support muscle function
Protein sits at the center, but nutrients also support muscle function. Vitamin D supports neuromuscular function. Magnesium supports contraction and energy metabolism. B vitamins support energy pathways. Food-first patterns usually cover the basics. When you suspect deficiency, confirm with a clinician and use targeted support.
resistance training principles for forty plus and beyond
Resistance training provides the strongest direct signal to keep muscle. It tells the body, “this tissue is still needed.” Research shows people can gain strength well past midlife. Progress may be slower, but it still happens with consistency.
progressive overload, but keep joints and tendons happy
Progressive overload means you increase challenge over time. You can increase weight, repetitions, sets, or difficulty. Do it gradually. Use controlled form. Avoid sudden jumps. Tendons often adapt more slowly than muscles. Smart pacing prevents setbacks.
train movement patterns that match real life
Focus on big patterns: squat, hinge, push, pull, carry, and rotate with control. These patterns support daily life. They also improve coordination and balance. Machines can help, too. Use whatever keeps training safe and consistent.
frequency: consistency beats extremes
Many adults do well with resistance training two to three times per week. Add light daily movement on most days. Recovery matters as much as training. If soreness lasts too long or sleep worsens, reduce volume and rebuild slowly.
recovery, sleep, and inflammation
Muscle adapts during recovery. Sleep supports repair, hormone regulation, and inflammation control. Poor sleep can blunt muscle protein synthesis and make training feel harder. It can also worsen insulin sensitivity.
simple sleep habits that support muscle
- keep a consistent sleep and wake time
- reduce bright light in the last hour before bed
- avoid heavy meals and alcohol too close to bedtime
- use a calming wind-down routine
low-grade inflammation can speed muscle decline
Chronic low-grade inflammation can push muscle toward breakdown. Ultra-processed diets, inactivity, poor sleep, and chronic stress can raise inflammatory signaling. A whole-food pattern, regular movement, and better sleep can help lower that burden over time.
who should be careful and common mistakes
Most adults can benefit from nutrition and strength work. Still, some people should move carefully and get guidance first.
who should seek professional guidance before big changes
- people with uncontrolled heart disease or unstable symptoms
- people with advanced joint disease or severe pain
- people with chronic kidney disease who plan a high-protein diet
- people with recent surgery or major balance problems
- people with unexplained weakness, rapid weight loss, or frequent falls
A clinician can help rule out hidden drivers, such as endocrine issues, neurological disease, medication effects, or malnutrition.
common mistakes that speed muscle loss and sarcopenia
- chasing weight loss without protecting muscle
- eating too little protein for long periods
- doing only cardio while avoiding resistance training
- training hard but sleeping poorly
- sitting for long blocks with no movement breaks
People often believe muscle loss is unavoidable. Research does not support that mindset. Muscle adapts when you give it a clear signal and enough resources.
frequently asked questions about muscle loss and sarcopenia
at what age does muscle loss and sarcopenia usually begin?
Muscle loss and sarcopenia can begin in midlife, often before symptoms feel obvious. The pace depends on activity, diet, sleep, health conditions, and inactivity periods. Early action tends to work better than late rescue.
is sarcopenia inevitable with aging?
No. Aging increases risk, but lifestyle strongly shapes outcome. Resistance training, adequate protein, enough energy intake, and good recovery can slow decline and support function across decades.
can walking alone prevent muscle loss?
Walking helps health and mobility, but it usually does not provide enough load to fully preserve muscle strength. Resistance training provides a stronger stimulus for muscle maintenance and strength.
does eating more protein automatically build muscle in older adults?
Protein helps, but it works best with resistance training. Aging muscle shows anabolic resistance. Training provides the key signal. Protein and energy provide the building blocks. Sleep supports recovery.
why does strength drop faster than muscle size?
Strength depends on nerves, coordination, and muscle quality. Aging can reduce motor unit efficiency and fast-twitch fiber function. You may lose power and balance before you see major size changes.
can muscle loss affect daily energy?
Yes. Muscle and mitochondria influence cellular energy production. When muscle quality drops and mitochondrial efficiency falls, fatigue can rise and recovery can slow.
final takeaway
Muscle loss and sarcopenia shape far more than appearance. They affect strength, balance, blood sugar control, and day-to-day energy. Aging plays a role, but daily habits often decide the speed of decline.
The most reliable path is a combined approach. Train muscle with resistance work. Eat enough high-quality protein. Avoid extreme dieting. Break up long sitting time. Protect sleep. This strategy may not stop aging, but it can support strength, mobility, and independence for years.
For a clinician-focused overview on strategies to slow muscle loss, you can also review:
Mayo Clinic: Slowing or reversing muscle loss.