How to Lower Cholesterol Naturally (LDL + Diet Plan)

✔
Medical Fact-Check: Verified against current Clinical Practice Guidelines and consensus reports from the National Institutes of Health and Harvard T.H. Chan School of Public Health .
Cholesterol is one of the most misunderstood markers in cardiovascular health. For decades, it has been portrayed as a simple villain. Yet modern cardiometabolic research shows a far more nuanced picture: cholesterol is biologically essential, but its balance, transport, and metabolism determine whether it protects your arteries or silently damages them.
If you are searching for how to lower cholesterol naturally, you are not alone. Millions of adults want effective, science-backed strategies that work before medication becomes necessary—or alongside it, under medical supervision. The good news is that current evidence suggests natural interventions can meaningfully reduce LDL cholesterol, improve HDL function, and lower cardiovascular risk when applied correctly and consistently.
This guide focuses on mechanisms, not myths. You will learn how cholesterol behaves in the body, which dietary and lifestyle levers truly matter, and how to use them strategically for measurable results.
expert summary
- Lowering cholesterol naturally is possible by targeting LDL production, absorption, and clearance through diet, activity, and metabolic timing.
- Not all cholesterol is harmful; particle type, oxidation, and transport (LDL vs HDL) matter more than total numbers alone.
- Consistency beats intensity: small, daily habits outperform extreme short-term interventions.
Safety alert: Natural strategies complement—but do not automatically replace—prescribed therapy. Anyone with established cardiovascular disease should act only in coordination with a healthcare professional.
table of contents
- what cholesterol really is and why it matters
- ldl, hdl, and triglycerides explained
- nutritional factors that influence cholesterol
- foods that lower cholesterol naturally
- bioavailability & practical usage
- lifestyle factors that amplify cholesterol reduction
- safety, side effects & contraindications
- frequently asked questions
- the final verdict
- actionable next steps
what cholesterol really is and why it matters
Cholesterol is a waxy, fat-like molecule synthesized primarily in the liver. It plays a critical biological role in cell membrane stability, hormone synthesis (including cortisol, estrogen, and testosterone), vitamin D production, and bile acid formation for fat digestion.
Approximately three quarters of circulating cholesterol is produced endogenously by the liver, while the remainder comes from dietary intake. This is why cholesterol management is not simply about avoiding certain foods—it is about modulating hepatic synthesis, intestinal absorption, and peripheral clearance.
Problems arise when cholesterol transport becomes dysfunctional. Excess cholesterol can accumulate within arterial walls, triggering inflammation, plaque formation, and eventually atherosclerosis.
[INSERT INFOGRAPHIC: cholesterol synthesis in the liver and transport through the bloodstream]
ldl, hdl, and triglycerides explained
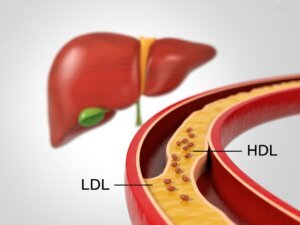
Understanding cholesterol begins with understanding its carriers. Cholesterol does not circulate freely in blood; it is packaged into lipoproteins.
| marker | primary role | health impact |
|---|---|---|
| LDL cholesterol | delivers cholesterol from the liver to tissues | excess LDL promotes arterial plaque formation |
| HDL cholesterol | returns cholesterol from tissues to the liver | protective when functional and sufficient |
| triglycerides | energy storage and transport | high levels amplify cardiovascular risk |
LDL cholesterol is not inherently “bad.” The risk depends on particle size, oxidation status, and how long LDL remains in circulation. Natural cholesterol-lowering strategies often work by improving LDL clearance and reducing oxidative stress.
Smart testing note: If you want a more precise risk picture, ask your clinician about non-HDL cholesterol, ApoB, and (when appropriate) lipoprotein(a). These markers can better capture atherogenic particle burden than total cholesterol alone.
nutritional factors that influence cholesterol
Dietary patterns influence cholesterol through multiple pathways: bile acid recycling, gut microbiota modulation, insulin sensitivity, and hepatic enzyme activity.
| nutrient | mechanism of action | effect on cholesterol |
|---|---|---|
| soluble fiber | binds bile acids in the intestine | lowers LDL cholesterol |
| unsaturated fats | improves lipid transport and receptor sensitivity | reduces LDL, supports HDL |
| plant sterols | compete with cholesterol absorption | decreases intestinal uptake |
| refined carbohydrates | increase insulin and hepatic lipogenesis | raises triglycerides and can worsen LDL patterns |
This is why cholesterol-friendly diets emphasize whole foods, fiber-rich plants, and metabolic stability rather than extreme fat avoidance.
Helpful external resources (evidence-based):
- National Heart, Lung, and Blood Institute (NHLBI): heart-healthy living
- NIDDK (NIH): weight management and metabolic health
- Harvard T.H. Chan: The Nutrition Source
- PubMed: search clinical studies on cholesterol and diet
foods that lower cholesterol naturally (what actually works)
Not all “healthy foods” lower cholesterol. The ones that do share specific biochemical actions: they increase bile acid excretion, reduce intestinal cholesterol absorption, improve LDL receptor activity, or decrease hepatic cholesterol synthesis.
| food category | key compounds | primary mechanism | cholesterol effect |
|---|---|---|---|
| oats & barley | beta-glucans | bile acid binding | lowers LDL |
| legumes | soluble fiber, polyphenols | reduced absorption, improved insulin response | lowers LDL & triglycerides |
| olive oil (extra virgin) | monounsaturated fats, polyphenols | improves LDL particle quality | reduces oxidation risk |
| nuts | plant sterols, unsaturated fats | competes with cholesterol absorption | modest LDL reduction |
| fatty fish | omega-three fatty acids | triglyceride reduction, anti-inflammatory | cardioprotective |
Important nuance: cholesterol reduction is dose-dependent. Small “sprinkles” of healthy foods do little. Consistent, daily intake at effective amounts produces measurable changes in blood markers.
[INSERT INFOGRAPHIC: cholesterol-lowering foods ranked by mechanism of action]
bioavailability & practical usage (how to apply this daily)
Knowing what lowers cholesterol is useless without knowing how to apply it. Timing, pairing, and consistency determine real-world results.
| strategy | best timing | why it works | practical tip |
|---|---|---|---|
| soluble fiber intake | with main meals | maximizes bile acid binding | start meals with oats or legumes |
| olive oil use | midday & evening | supports lipid transport | replace refined oils completely |
| physical activity | daily, post-meal preferred | enhances LDL clearance and triglyceride handling | ten to twenty minute walks |
| evening light meals | three hours before sleep | reduces nocturnal lipogenesis in susceptible people | avoid late refined carbs |
Pro-tip: Post-meal walking often improves triglyceride clearance more effectively than fasted exercise for adults with insulin resistance patterns.
lifestyle factors that amplify cholesterol reduction
daily movement and circulation
Regular movement increases lipoprotein lipase activity and supports LDL receptor expression in the liver. Even low-intensity walking improves lipid profiles when performed consistently.
sleep and circadian rhythm
Short or irregular sleep disrupts hepatic cholesterol metabolism and can worsen appetite regulation, visceral fat distribution, and insulin sensitivity—all of which can worsen lipid patterns over time. Stable sleep timing supports hormonal regulation and lipid balance.
stress regulation
Chronic cortisol elevation promotes visceral fat accumulation and worsens lipid profiles in many individuals. Stress management can indirectly but meaningfully support cholesterol control by improving metabolic stability and reducing inflammatory load.
[INSERT INFOGRAPHIC: lifestyle factors influencing cholesterol metabolism]
safety, side effects & contraindications
Natural does not mean risk-free. While lifestyle-based cholesterol reduction is generally safe, certain populations require caution.
- established cardiovascular disease: lifestyle strategies should complement, not replace, medical therapy.
- very high LDL levels: natural approaches may be insufficient alone; delayed treatment can increase long-term risk.
- rapid dietary changes: high fiber increases can cause bloating, gas, or discomfort at first; increase gradually and hydrate.
- supplement caution: “cholesterol supplements” can interact with medications or be inappropriate for certain conditions; discuss with a clinician.
Red flags to discuss promptly with a clinician: strong family history of early heart disease, very high LDL, diabetes, kidney disease, or symptoms suggestive of cardiovascular disease.
frequently asked questions (snippet optimized)
can cholesterol really be lowered naturally?
Yes, current clinical evidence suggests that LDL cholesterol can be reduced naturally by targeting diet composition, daily movement, sleep stability, and metabolic timing, particularly in individuals without advanced cardiovascular disease, often producing clinically meaningful improvements within several weeks. Results vary based on baseline risk, genetics, and adherence.
how long does it take to see results?
Most people begin to see measurable changes in cholesterol markers within four to eight weeks when evidence-based dietary and lifestyle strategies are applied consistently, although maximal benefits may require several months of sustained adherence. Retesting after about eight weeks is a practical checkpoint.
is medication always necessary for high cholesterol?
Medication is not always required, especially in mild to moderate elevations without additional risk factors, but individuals with established heart disease or very high LDL levels should never discontinue prescribed therapy without medical guidance. Your overall risk profile determines the safest plan.
are eggs and dietary cholesterol dangerous?
For most individuals, dietary cholesterol from whole foods such as eggs has a limited effect on blood cholesterol compared to overall dietary pattern, fiber intake, and refined carbohydrate load, though individual responses can vary. If LDL rises significantly, personalize intake with your clinician.
the final verdict
Lowering cholesterol naturally is not about extremes. It is about understanding how cholesterol moves through the body and using food, movement, sleep, and timing to restore balance.
For many adults, these strategies are sufficient to meaningfully reduce LDL cholesterol and cardiovascular risk. For others, they serve as a powerful foundation that enhances the effectiveness of medical therapy under professional supervision.
Internal reading (recommended):
actionable next steps
- review your lipid profile with a healthcare professional (and ask whether ApoB or non-HDL would add clarity)
- build meals around soluble fiber and unsaturated fats most days of the week
- commit to daily post-meal movement, especially after the largest meal
- stabilize sleep and meal timing for metabolic consistency
- retest key markers after about eight weeks and adjust strategically